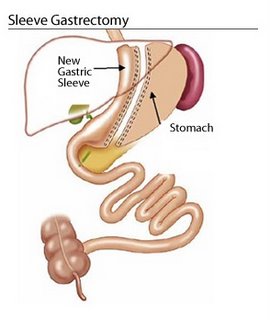
ASMBS: Laparoscopic adjustable gastric banding less effective than gastric bypass and sleeve gastrectomy
Dallas, TX
Patients who underwent laparoscopic adjustable gastric banding achieved less weight loss and less improvement in comorbid conditions than those who had gastric bypass or sleeve gastrectomy.
Slightly more than half of gastric banding patients lost more than 50% of excess weight after five years compared with more than 90% of patients who underwent laparoscopic Roux-en-Y gastric bypass, Diego Awruch, MD, reported at the American Society of Metabolic and Bariatric Surgery.
Surgical failure, defined as less than 50% excess weight loss, was almost six times more common with gastric banding.
"Laparoscopic adjustable gastric banding was associated with fewer complications, but the percent weight loss at one and five years was inferior to laparoscopic Roux-en-Y gastric bypass," said Dr. Awruch, of Pontificia Universidad Catolica in Santiago, Chile.
"Surgical failure occurred in more than 40% of patients who underwent gastric banding, and 16% of the patients required surgical revision of the initial procedure," he said.
Similar disparities in weight loss occurred in the comparison of gastric banding and sleeve gastrectomy.
Across the entire range of body mass index (BMI), laparoscopic sleeve gastrectomy led to greater weight loss, said David Schumacher, MD, of Wright State University in Kettering, Ohio.
Dr. Awruch reported outcomes for 91 patients treated with laparoscopic Roux-en-Y surgery and 62 who underwent gastric banding from 2001 to 2003.
Five-year follow-up was available for 73.6% of the gastric bypass patients and 91.5% of the gastric banding patients.
Comparison of baseline characteristics showed that bypass patients weighed significantly more (106.4 versus 97.6 kg, P<0.001) and had a significantly higher BMI (39 versus 35, P<0.001).
Gastric bypass was associated with a higher rate of early complications (14.2% versus 1.6%, P=0.009). In addition, nine bypass patients required reoperation or endoscopic dilatation compared with one patient in the banding group.
Late complications occurred in 37.3% of bypass patients compared with 27.4% of gastric banding patients, but the difference did not reach statistical significance. A higher proportion of gastric banding patients required reintervention (23 of 62 versus 20 of 91).
Percent weight loss at five years averaged 92.9% with gastric bypass compared with 59.1% with gastric banding (P<0.001).
Dyslipidemia, insulin resistance, hypertension, and type 2 diabetes improved or resolved in 80% to 100% of bypass patients compared with 20% to 40% of the gastric banding group.
At five years, 94% of bypass patients and 54.4% of gastric banding patients had maintained >50% excess weight loss.
Dr. Schumacher reported outcome data for 104 patients who underwent laparoscopic sleeve gastrectomy and 227 who had gastric banding from January 2006 through August 2008. Follow-up data were 99% as of January 2009.
Among patients followed for at least 18 months (about half of the total), weight loss averaged 133.82 lb in the sleeve group versus 58.93 lb in the banding group.
For the same time interval, excess weight loss averaged 55.54% with sleeve gastrectomy versus 38.65% with banding.
Stratification of patients by baseline BMI showed that sleeve patients had a greater excess weight loss in patients with BMI more than 50 (50% versus 33%), 40 to 49 (68% versus 40%), and less than 40 (90% versus 43%).
Readmission rates were 6% of sleeve gastrectomy patients and 1.3% with gastric banding. One patient (0.96%) in the sleeve group required reoperation compared with 19 (8.4%) gastric banding patients.
"Laparoscopic sleeve gastrectomy appears to allow greater weight loss in all BMI classifications over time with fewer reoperations," said Dr. Schumacher. "The most efficient weight loss occurred in the lowest BMI classification.
"Laparoscopic sleeve gastrectomy can be used effectively as a primary operation in any weight classification, achieving a greater than 50% excess weight loss in all BMI subsets."
Labels: gastric bypass revision, gastric bypass surgery, Lap-Band surgery, sleeve gastrectomy